Table of Contents
- Perovial® arrives in the Canary Islands
- What is Peyronie's disease?
- Why the acute phase is key
- How Perovial® works
- What is the treatment like?
- Security and who it is for
- How we accompany you in GUA
- Request your assessment
Perovial® in the Canary Islands: a new option for treating Peyronie's disease in its acute phase
At GUA Urology and Andrology Clinic, we have incorporated Perovial® (IBSA), becoming the first clinic in the Canary Islands to offer this intraplaque approach with hyaluronic acid indicated for the acute (active) phase of Peyronie's disease.
The goal is to open up a pathway for early intervention in a condition that can cause pain, penile curvature, and a significant impact on sexual life and emotional well-being.
What is Peyronie's disease?
Peyronie's disease (or penile induration) is an acquired condition in which a fibrous plaque forms in the tunica albuginea. This plaque reduces the elasticity of the tissue and can result in:
- Penile curvature during erection
- Pain, especially at the beginning
- Deformity or feeling of "tightness"
- Difficulty with penetration
- In some cases, erectile dysfunction
The acute phase: the "window" in which we can help the most
In consultation, we see that the timing of seeking treatment matters. The disease usually has an acute (active) phase, in which there is inflammation and symptoms such as pain, and a stable (chronic) phase where the deformity becomes established.
The acute phase is important because:
- This is when there may be pain during erection and recent changes.
- It is a stage in which we seek to limit progression and preserve function.
"The acute phase is a key moment: if we intervene early, we can try to slow progression, relieve pain, and preserve function." Dr. María Fernanda Peraza Godoy (GUA)
What is Perovial® and how does it work?
Perovial® is a medical device containing 0.8% highly purified hyaluronic acid. It is indicated for the treatment of Peyronie's disease in its acute phase.
According to its documentation, hyaluronic acid may contribute to:
- Soften the plaque (due to its ability to retain water)
- Promote tissue remodeling
- Provide antioxidant and antifibrotic effects that can help limit progression at this stage
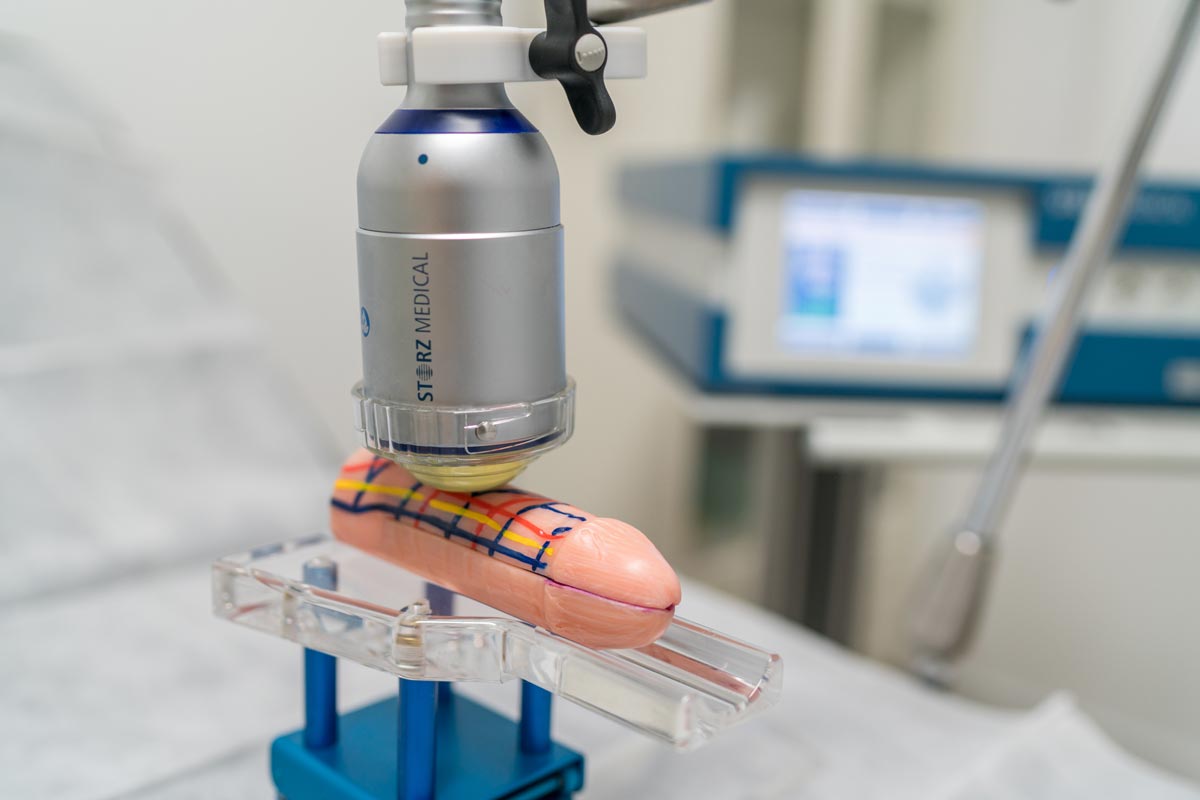
What is treatment with Perovial® like?
The treatment is performed by qualified personnel using intra-plaque injections. It is usually prescribed on a weekly basis for 10–12 weeks, adjusting the volume according to the plaque and medical criteria.
After the injection, it is usually recommended to avoid sexual activity and intense physical activity for 24–48 hours.
Security and who it is for
As with any intralesional treatment, temporary local effects may occur (e.g., pain, redness, swelling, or bruising at the injection site).
Expert assessment is key because Perovial® is not indicated in all cases (e.g., calcified plaques or some complex deformities described in its documentation).
How we support you at GUA (Las Palmas de Gran Canaria)
At GUA Urology and Andrology, we are committed to a conservative and personalized approach whenever possible, with expert diagnosis, follow-up, and selection of the most appropriate therapy for each phase.
The incorporation of Perovial® is another step toward bringing current treatments to the Canary Islands, avoiding travel and expanding options for early intervention when indicated.
Request your assessment at GUA
If you have noticed pain during erection, recent curvature, or changes in the shape of your penis, early assessment can make all the difference.
Frequently asked questions about Perovial® and Peyronie's disease
What is Perovial®?
Perovial® is a medical device composed of 0.8% hyaluronic acid indicated for the treatment of the acute (active) phase of Peyronie's disease. It is administered by intraplaque injection performed by an experienced urologist.
For which stage of Peyronie's disease is it indicated?
It is indicated for the acute or active phase, when the plaque is not yet calcified and there may be pain during erection or recent changes in curvature. It is not indicated in the chronic phase with calcified plaques.
How does hyaluronic acid work in Peyronie's disease?
Hyaluronic acid has the ability to retain water, promoting tissue hydration and elasticity. It also has antioxidant and antifibrotic properties that can help limit plaque progression in the active phase.
What is treatment with Perovial® like?
The usual protocol consists of weekly intraplaque injections for approximately 10–12 weeks. The volume is adapted to the size of the plaque and the physician's criteria. The procedure is performed in the doctor's office, usually under local anesthesia.
Does the injection hurt?
It is performed under local anesthesia, so the procedure is well tolerated. After the injection, mild discomfort, swelling, or a small bruise may appear, but these are usually temporary.
Does it have any side effects?
The most common side effects are local and mild: pain at the injection site, redness, swelling, or bruising. It is essential that the treatment be performed by a qualified specialist.
Is it effective for calcified plaques?
No. Perovial® is not indicated for calcified plaques (stable chronic phase) or certain complex deformities, such as some "hourglass" deformities. That is why a prior specialist assessment is essential.
Can you avoid surgery?
In some patients, early treatment in the acute phase can help limit progression and preserve function. However, each case must be assessed individually to determine whether conservative management is sufficient or whether another approach may be required in the future.