By Dr. Nicolás Nervo – Specialist in Urology and Andrology.
Transperineal fusion prostate biopsy is currently one of the most accurate and safest techniques for diagnosing prostate cancer. At GUA Urology and Andrology in Las Palmas de Gran Canaria, we perform this advanced biopsy to obtain a reliable diagnosis, minimize risks, and offer a personalized medical approach.
Table of Contents
- Why is it important to talk about transperineal fusion prostate biopsy today?
- What is a transperineal fusion prostate biopsy?
- How is it done step by step?
- Patient preparation and recovery
- Advantages of transperineal fusion prostate biopsy compared to conventional biopsy
- In which cases is transperineal fusion prostate biopsy indicated?
- Risks and common side effects
- Transperineal fusion biopsy at GUA Urology and Andrology
- Make an appointment today
Why is it important to talk about transperineal fusion prostate biopsy today?
Prostate cancer is the most common tumor in men. It is estimated to affect approximately 1 in 9 men throughout their lives and, in many cases, does not produce symptoms in the early stages. That is why it is so important to have accurate and early diagnostic methods.
Transperineal fusion prostate biopsy has become one of the most advanced techniques available in Europe today for safely and reliably confirming or ruling out prostate cancer. It allows for better localization of suspicious lesions, targeted sampling, and reduced risks associated with traditional biopsies.
If you would like more general information about prostate cancer, you can consult our clinic's specific page on
prostate cancer or visit patient resources such as the Spanish Association Against Cancer and the European Association of Urology.
What is a transperineal fusion prostate biopsy?
Transperineal fusion prostate biopsy is a diagnostic technique that combines two types of imaging:
- A multiparametric magnetic resonance imaging (MRI) scan of the prostate, performed previously.
- A real-time transperineal ultrasound.
Using an image fusion system, both tests are integrated to create a three-dimensional (3D) reconstruction of the prostate. Using this 3D image, the urologist can identify suspicious areas with great precision and direct the needle exactly to the points where a clinically significant tumor is most likely to be found.
In addition, micro-ultrasound technology is used, which provides superior resolution compared to conventional ultrasound. This facilitates the detection of small or clinically relevant lesions, increasing the overall reliability of the biopsy.
If you would like to see the technical details of this test at our clinic, please visit
transperineal fusion prostate biopsy.
How is it done step by step?
The biopsy is performed transperineally, accessing the prostate through the skin of the perineum (the area between the scrotum and the anus), without passing through the rectum. This avoids contact with the intestinal flora and reduces the risk of infection.
The usual procedure includes:
- Sedation and positioning of the patient: the patient is sedated, comfortable, and pain-free.
- Live ultrasound: An ultrasound is performed while the patient is sedated.
- Merging ultrasound with previous magnetic resonance imaging: the system integrates both images.
- 3D reconstruction of the organ: a three-dimensional model of the prostate is generated.
- Obtaining samples: biopsy cylinders are taken with millimeter precision from the suspicious areas.
The total duration of a transperineal fusion prostate biopsy is usually 20 to 40 minutes, depending on the complexity of each case and the number of samples required, in accordance with standard times in advanced clinical practice.
Patient preparation and recovery
Preparation for a transperineal fusion prostate biopsy is usually minimal. In general, the following is recommended:
- Fasting for a few hours before the procedure, due to sedation.
- Adjustment of anticoagulant medication when appropriate, always under medical supervision.
- Occasionally, antibiotic prophylaxis according to individual clinical criteria.
After the test, the patient can resume normal activities within a short period of time, avoiding strenuous activity for a few days. It is normal to experience mild discomfort in the perineal area or small amounts of blood in the urine or semen, which are usually temporary.
Advantages of transperineal fusion prostate biopsy compared to conventional biopsy
Transperineal fusion prostate biopsy offers significant advantages over traditional transrectal biopsy:
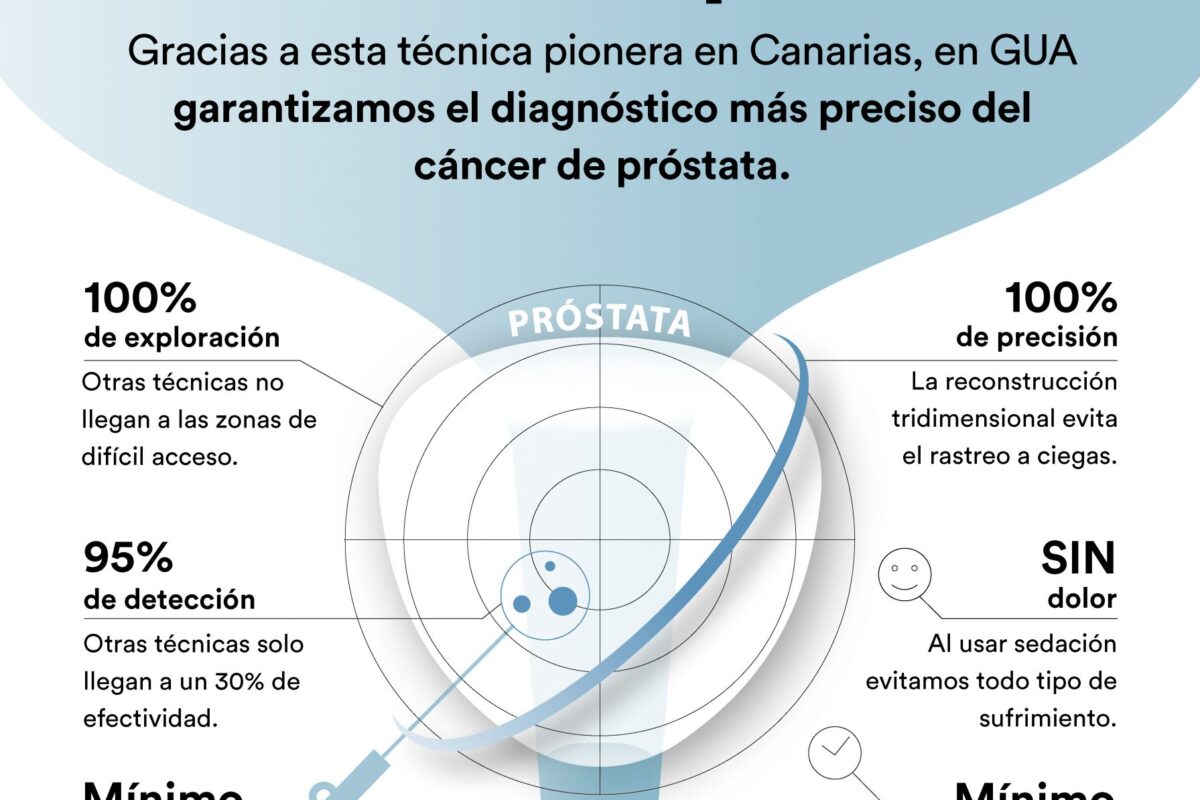
- Greater diagnostic accuracy: detection capability is close to 95%, compared to around 30% for other techniques.
- Complete prostate examination: allows areas that are difficult to access with other techniques, such as the anterior zone, to be examined.
- Lower risk of infection: since it does not pass through the rectum, the possibility of prostatitis, urinary tract infections, or sepsis is reduced.
- Painless procedure: performed under sedation, providing a comfortable experience.
- Greater safety and rapid recovery: fewer complications and a quick return to daily life.
- 3D image fusion: the urologist directs the samples to the areas that are truly suspicious, avoiding "blind" biopsies.
- Fewer punctures: by focusing on areas of interest, fewer cylinders may be required to reach a diagnosis.
In summary, this technique significantly increases the probability of detecting significant tumors while reducing risks and discomfort for the patient.
In which cases is transperineal fusion prostate biopsy indicated?
Transperineal fusion prostate biopsy is a diagnostic tool, not a general screening test for healthy populations. It is particularly indicated when prostate cancer is suspected, for example in:
- Elevated or rising PSA (prostate-specific antigen).
- Abnormal findings on digital rectal examination, such as irregular prostate, presence of nodules, or hardening.
- Suspicious lesions on multiparametric prostate magnetic resonance imaging.
- Need to expand or confirm previous studies when other tests have been inconclusive.
It is not used as a preventive technique in men without symptoms or risk factors, but it does play a key role in patients who have already shown warning signs or abnormalities in initial tests.
Risks and common side effects
Like any medical procedure, transperineal fusion prostate biopsy is not entirely risk-free. However, the transperineal approach has been shown to have a lower complication rate than transrectal biopsy.
By not passing through the rectum, the likelihood of the following is significantly reduced:
- Prostatitis.
- Urinary tract infections.
- Sepsis (severe generalized infection).
The most common side effects following transperineal fusion prostate biopsy include:
- Discomfort or mild pain in the perineal area.
- Presence of blood in urine or semen for a few days.
These symptoms are usually mild and self-limiting. After the procedure, the patient receives clear instructions on when to contact the medical team if they have any concerns.
Transperineal fusion biopsy at GUA Urology and Andrology
Transperineal fusion prostate biopsy requires advanced equipment and a specialized medical team. Not all centers have image fusion systems, micro-ultrasound technology, and specific experience in this type of procedure.
At GUA Urology and Andrology, in Las Palmas de Gran Canaria, we combine:
- Image fusion systems (magnetic resonance imaging + ultrasound).
- High-resolution micro-ultrasound.
- A team of urologists with extensive experience in precision oncological urology.
Our goal is to offer you:
- The most accurate diagnosis possible when prostate cancer is suspected.
- A safe, painless procedure with quick recovery.
- Prompt communication of results, which are usually available within 48 hours.
We integrate the biopsy information with the rest of your tests and, if necessary, we evaluate advanced treatment options. You can learn more about our team at
GUA team and continue to stay informed at
urological health blog.
If you have been informed of an elevated PSA, have been recommended a transperineal fusion prostate biopsy, or are seeking a second opinion, at GUA Urology and Andrology we can help you.
Take the next step toward an accurate and reliable diagnosis:
"An accurate diagnosis is the first step toward successful treatment. At GUA Urology and Andrology, we accompany you every step of the way."